April 21, 2014
Preparing Mothers for Breastfeeding after a Cesarean - The Educator's Role
By: Sharon Muza, BS, LCCE, FACCE, CD/BDT(DONA), CLE | 0 Comments
By Tamara Hawkins, RN, MSN, FNP, IBCLC, CHHC, LCCE
April is Cesarean Awareness Month (CAM). In a post earlier this month, I shared my favorite websites for birth professionals to learn and share with students and clients about cesarean prevention, recovery, vaginal birth after cesarean along with a fun quiz to test your knowledge about cesarean and VBAC information. Today, as Lamaze International continues to recognize CAM, LCCE and IBCLC Tamara Hawkins shares information on how professionals can help prepare women who will be breastfeeding after a cesarean to get off on the right track for a successful breastfeeding relationship. - Sharon Muza, Science & Sensibility Community Manager.
Working in New York City, I see many women who have given birth to their babies via cesarean section. Most hospitals in my area have a cesarean rate close to 40% and 30% of those births are primary cesareans. April is Cesarean Awareness Month and I wanted to discuss cesarean birth and breastfeeding. As both a Lamaze Certified Childbirth Educator and an International Board Certified Lactation Consultant, I work with women both before and after a cesarean birth. I meet mothers who could have prevented many lactation issues if equipped with a few practices to get breastfeeding off to a good start after a cesarean birth. I want to share some practical teaching tips on preparing a mother to successfully breastfeed after having a cesarean birth. In a childbirth class, it is important to give anticipatory guidance to mothers in class who are preparing to birth about the realities of breastfeeding after a cesarean.
I recommend discussing breastfeeding after cesarean births in all portions of your childbirth class; labor and birth, newborn care and breastfeeding classes, in order to cover different aspects of breastfeeding initiation. During the labor and birth variations class, discuss how cesarean births affect baby and mother physically and emotionally. Provide tips on how to get through the first days in the hospital such as skin to skin, rooming in, explain the normalcy of cluster feeding and give breastfeeding support resources for the mother to use once she returns home. I find giving a wealth of well researched information in class will not help a mother who may be having breastfeeding trouble several weeks later after the baby has arrived. In newborn care and/or breastfeeding class, provide additional details: latch, positioning, signs of hunger, feeding length and times, cluster feedings, care for engorgement and sore nipples. Supplement with your list of resources.
Many birth professionals report cesarean births as a common reason for delayed Lactogenesis I. I like to lay out solutions for common concerns and problems that arise for mothers when breastfeeding after a cesarean. These solutions include care for the areola/nipple complex, swelling, positioning and latch techniques, anticipating frequent feedings, feeding a sleepy baby, and caring for engorged breasts.
Solutions and Teaching Points
Insufficient glandular tissue and low milk supply
I have seen an explosion of mothers who have insufficient glandular tissue and low milk supply. During class discussions about baby's first feeding, explain normal breast changes to expect during pregnancy such as prominent veining, dark areola/nipple complex, growth of about one cup size in breast tissue, and tenderness. These changes indicate the process of Lactogenesis Stage I - when the epithelial cells of the breasts begin to convert to milk secreting cells under the influence of the hormone prolactin. When mothers have no or very little breast growth during pregnancy this indicates a deficiency in stage I of lactogenesis. Often, this is why a mother may have trouble with milk supply and not just because she had a cesarean. It is important we make a distinction in this for the mother because if the mother is blaming herself for an unplanned cesarean and then believes the cesarean birth caused the low milk supply it can cause undue distress. I typically just present the expected breast growth information and state, "If you have not had any changes, feel free to reach out to me or speak with your health care provider about your concerns." When a mother is empowered with anticipatory guidance, it can help her make solutions to adequately feed her baby at birth, build her milk supply and find appropriate breastfeeding support. Even if she has a cesarean, she should not expect low milk supply unless she has the markers of IGT.
Creative positioning and latch techniques
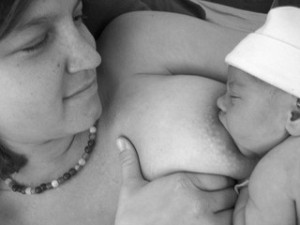
© http://flic.kr/p/5f29EK
We cannot expect a mother to sit straight up in a chair to nurse after a cesarean and we have to model positions to help mothers understand how to nurse laying back, in football positions and cross cradle. The side lying position for mothers who gave birth by cesarean can be hard as the mother can experience pulling on her incision as she is trying to roll on to her side. Additionally, as she is laying in the side lying position, there can be pain, and some babies' legs are long and can kick the incision. Depending on the available space where I teach, I can get on the floor and demonstrate how to hold the baby in multiple positions simulating being in a bed. I also discourage the use of "breastfeeding pillows." They tend to not fit well around a mother in bed. If a mother is in a chair she's liable to lean too far over to reach the baby who is resting on the pillow. It's best to teach good posture in classes to prevent maternal back and neck discomfort and demonstrate having the baby up close to mother's abdomen and breast to affect a deep latch.
Frequent feeding
Parents will receive many "tips" about breastfeeding after a cesarean delivery. Every nurse, health care provider, lactation consultant/counselor, mother, sister and friend will tell her something different about when to feed her baby. It is the role of the childbirth educator to prepare them for frequent feeds and give rationales as to why feeding a baby frequently is important. Rather than stating a set "frequency" such as feed every 2-3 hours, I want them to understand the newborn's normal pattern of sleep and wakefulness and how this influences their feeding behaviors. Mothers may be drowsy after a cesarean birth, particularly if the surgery followed a long labor. They may also be in pain. Pain medication, while necessary for good pain management after surgery, can also contribute to a mother feeling sleepy. Holding her baby skin to skin will help the mother connect with her baby and relax. Both mother and baby need to be relaxed to get breastfeeding off to a good start. Explain to mothers during class that babies may want to nurse within the first hour and to wait for those cues: rooting, hands to mouth and suckling. Babies are often sleepy after cesarean births, especially if mother was pushing, had been treated with magnesium for pre-eclampsia or had been through a long induction. When a baby does not feed as often as anticipated, this will of course upset the mother and can lead to delayed Lactogenesis II.
Educators have to set expectations properly. Working on a time line, I discuss, breastfeeding in the operating room during the cesarean repair and in the recovery room. When partners are in class, teach them how to place the baby skin to skin with mom and support the baby if the mother's arms or hands are restricted with blood pressure cuffs and IV lines. Discuss hand expression for those sleepy babies who are not rooting within 45 minutes of birth. Dr Jane Morton has a fantastic video illustrating how to express colostrum by hand. This is especially important for babies born to a mother with gestational diabetes, as these babies tend to be at risk for low blood sugar and formula supplementation.
If the baby has to go to the nursery before breastfeeding has been established, we discuss delaying the newborn bath and the rationale. When babies get a bath, not only is the vernix and amniotic fluid (which is a familiar taste to the baby) washed off, the baby will most likely cry, a lot, and fall into a deep sleep making it harder to wake for a feeding. Also, many babies are kept for a longer time in the nursery to warm up after the bath delaying skin to skin and breastfeeding. If the baby has not breastfed in the operating or recovery room, suggest the parents ask for the bath to be delayed until the next day and expect the baby to be on contact precautions. That means there may be a sign on the bassinet alerting care providers to wear gloves when caring for the baby.
Moving along the timeline, we move right into newborn sleep-wake patterns and cluster feedings. I tell them the baby is not born knowing there is a clock on the wall. There is no magic formula that says the baby should be fed 8x/day or every 3 hours or even for 15 minutes on the breast. Expect the baby to nurse 45 minutes every hour for four to five hours straight. That's when you will really get their attention and can again discuss normal baby routines, colostrum volumes and the size of the newborn stomach.
Dealing with a sleepy baby
Babies born via cesarean can be sleepy for many reasons; exposure to magnesium sulfate and analgesia, long labors, and long second stage to name a few reasons. These babies need to be fed one way or another. Teach clients how to hand express and feed their baby at the breast. Holding the baby close to the breast, hand express 20 drops from each breast and rotate twice between each breast. Approximately 80 drops equal a teaspoon. This is the estimated amount the baby will take in during breastfeedings on day one and two of life. The mother can hand express directly into the baby's mouth or into a spoon. I prefer a soft baby spoon as a plastic spoon can be sharp on the edges. Hand expression can prevent serious engorgement and increase likelihood of normal Lactogenesis II by stimulating release of prolactin.
Dealing with engorgement
Mothers that get engorged after a cesarean sometimes are dealing with breasts that are extremely edematous. It is important to discuss the difference of being engorged with milk versus engorged with interstitial fluid or swelling. At the time I cover the topic of cesareans in the childbirth class, I differentiate the two by describing how the breasts feel under both circumstances. I describe the breasts as feeling like a bag of marbles when it is full of breast milk and like an overfilled water balloon when it is just interstitial fluid. The care plan for each type of engorgement is a bit different. To start, emphasize on demand feedings to prevent buildup of fluid and discuss the use of Reverse Pressure Softening to remove local swelling in the areolar/nipple complex to affect a deep latch.
Breasts that appear swollen and feel soft like a water balloon need hand expression to get the milk flowing and to keep the areola soft. No application of heat is warranted with this type of swelling. Warm compresses can cause blood and lymphatic vessels in the breast to dilate and release more fluid. The goal is to reduce the swelling. After every feeding, application of cool compresses to the breasts is best. Cold therapy slows circulation, reducing inflammation, muscle spasm, and pain. The goal here is to keep the areola soft to prevent pressure building up around the milk ducts and prevention of milk flow.
Breasts that are hard with palpable alveoli are full of milk. The mother can once again use hand expression to get the milk flowing and will benefit from warm compresses to the breast for about 5-10 minutes before feeding. If her milk begins to leak, than the warmth is a good tool. If the milk does not begin to leak out, that is an indication that interstitial swelling is present and heat should not be used. Only cool compresses after feeding and/or pumping should be used in this situation.
Mothers that have cesarean births are very vulnerable to the hardships that come along 3-4 days after the birth including sore and swollen breasts, possible low milk supply and general recovery complaints that are associated with major abdominal surgery. Giving anticipatory guidance to succeed with breastfeeding amongst these possible issues and challenges are important to help mothers gain the confidence to succeed in making breastfeeding work.
After birth, a mother may have less support in her postpartum room and at home. She may even be alone most of the time during breastfeeding. After her labor and birth, it is likely she will not be able to access information stored in the left side of her brain if she is having breastfeeding difficulties coupled with fatigue and pain from birth. She will still reach out and ask questions. Very likely her first sources will be an online chat room, on a Facebook page or on a website somewhere. Childbirth educators should provide specific resources to find breastfeeding information. Share local breastfeeding and cesarean birth support groups along with the contact information for breastfeeding professionals during your childbirth classes.
I recognize that there is a lot of work to do in the birth world to bring down the cesarean birth from the current 32.8%. We can inform our students and clients with information to keep breastfeeding as normal as possible if a cesarean birth should occurred. It is our responsibility in the classroom to give our clients those tools to help them succeed in breastfeeding no matter how they give birth.
What information do you share with your clients about cesarean birth and successful breastfeeding? How do you prepare them for possible breastfeeding hurdles after a cesarean birth?
About Tamara Hawkins
 Tamara Hawkins, RN, MSN, FNP, IBCLC, CHHC, LCCE is the director of Stork and Cradle, Inc offering Prenatal Education and Breastfeeding Support. She graduated with a BSN from New York University and a MSN from SUNY Downstate Medical Center. She is a Family Nurse Practitioner and has worked with mothers and babies for the past 16 years at various NYC medical centers and the Elizabeth Seton Childbearing Center. Tamara has been certified to teach childbirth classes since 1999 and in 2004 became a Lamaze Certified Childbirth Educator and an International Board Certified Lactation Consultant. Follow Tamara on Twitter: @TamaraFNP_IBCLC
Tamara Hawkins, RN, MSN, FNP, IBCLC, CHHC, LCCE is the director of Stork and Cradle, Inc offering Prenatal Education and Breastfeeding Support. She graduated with a BSN from New York University and a MSN from SUNY Downstate Medical Center. She is a Family Nurse Practitioner and has worked with mothers and babies for the past 16 years at various NYC medical centers and the Elizabeth Seton Childbearing Center. Tamara has been certified to teach childbirth classes since 1999 and in 2004 became a Lamaze Certified Childbirth Educator and an International Board Certified Lactation Consultant. Follow Tamara on Twitter: @TamaraFNP_IBCLC
Tags
Breastfeeding Childbirth education Cesarean Awareness Month IBCLC Labor/Birth Maternal Infant Care CAM Tamara Hawkins